By: Mary Gipson, PhD, ARNP
It has been estimated that as many as 50 percent of the American population has the virus that causes these painful mouth sores. But not everyone who has the virus develops the sores. To better understand how this virus affects people, let’s take a closer look at this condition.
The virus that causes cold sores is one of two types of the Herpes Simplex Virus. It is also called HSV-1. As you would guess, the second type is referred to as HSV-2. The two types differ in the strain of the virus and area of the body the virus usually affects. HSV-1 most often affects the oral areas while HSV-2 usually affects the genital areas. For the purpose of this article, we will focus on HSV-1.
HSV-1 is a chronic, incurable, lifelong infection. Infection with HSV-1 occurs when a person is exposed to the virus from someone else who already has it, through close contact with oral secretions. A person is most contagious when they have active mouth sores, although this is not necessary to spread the virus.
HSV-1 infection occurs in three stages:
Stage One
Upon exposure, the virus enters the body through small miniscule breaks in the skin or mucous membrane. The person may develop a fever and mouth sores during this stage.
Stage Two
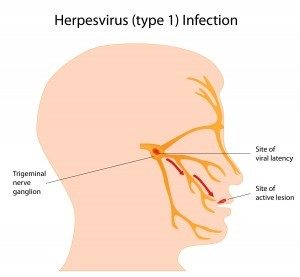
The virus searches out a nerve, usually the trigeminal nerve, to which it can attach (see illustration). Here the virus remains inactive until a stressful event such as fatigue or illness reactivates it.
Stage Three
The reactivated virus surfaces to the skin, resulting in blisters that eventually crust and heal. The virus then goes back into hiding only to resurface again with the next stressful event.
People who develop mouth sores from HSV-1 usually experience a tingling, burning sensation on or close to their lips or inside their mouth prior to the appearance of an often painful cluster of bumps and blisters on a red base. Once these blisters rupture, they crust and heal over in one to two weeks, usually without leaving a scar.
Tori
Working with my students just a few weeks ago in the clinical setting, we encountered a young woman named Tori who had a cluster of blisters on her lip and appeared to have HSV-1 in Stage Three.
Tori is a 19-year-old college student who came to the clinic seeking information on treating her cold sores. She told us that she first started getting cold sores on her lower lip around the age of 15, but that they have been reoccurring with greater frequency since she started college last fall. Tori told us that the blisters are painful, but more important to her were her feelings of embarrassment every time a sore developed.
Based on Tori’s history and the appearance of the blisters, she was diagnosed with HSV-1. More extensive testing through a skin sample can be done to confirm, but most often the diagnosis of HSV-1 is based on a person’s history and the appearance of the sore. We prescribed the oral antiviral acyclovir to treat symptoms and promote faster healing.
Acyclovir interrupts the replication of viral DNA and discourages new blister formation. In addition, we recommended to Tori that she use over-the-counter medications for pain and cold compresses for itching. She was also advised to not touch the blisters, to wash her hands frequently, and to avoid exposing others by kissing or the sharing of tableware, personal products, etc. before her blisters and lesions healed. Most importantly, we reviewed with Tori ways to prevent reoccurrences of the oral sores through personal stress management, good nutrition, and healthy living.

Nursed to Health is a recurring feature in the The Florida Times-Union. Jacksonville University Keigwin School of Nursing faculty discuss symptoms, diagnoses, and treatments based on patient cases handled by instructors, students, and alumni. Today’s column is by Keigwin School of Nursing Professor Mary Gipson, who specializes in adult health, critical care, and pharmacology within JU’s Brooks Rehabilitation College of Healthcare Sciences.
 Wave Magazine Online Jacksonville University News Hub
Wave Magazine Online Jacksonville University News Hub