President Dwight Eisenhower, former pro golfer Al Geiberger, former all-pro Green Bay Packer Jerry Kramer, the late U.S. Speaker of the House Thomas “Tip” O’Neill and Olympic gold medalist and pro golfer Babe Zaharias all had something in common — they had an ostomy, a surgically created opening in which a portion of the colon or ureter is removed, and the remaining portion is brought to the surface of the abdominal wall.
When the colon is involved, it is call an intestinal diversion or colostomy. When the ureter is involved, it is called a urinary diversion or urostomy. There are many reasons this procedure may be performed, with intestinal cancers and diverticulosis most common for intestinal diversion and bladder cancer for urinary diversion.
The typical reaction of having an ostomy is at first shock, particularly just after the surgery, even if the surgeon and nursing staff have prepared the patient. The second stage is denial, with refusal to look, much less touch, the ostomy and appliances. The third stage is an acknowledgment that one’s life will continue, followed by the adaptation of lifestyle modifications to enhance one’s self-worth and abilities.
Here’s a look at a recent patient who had a colostomy.
WILLIAM
William, 52, scheduled his colonoscopy after several exacerbations of diverticulitis with bleeding. He was then referred to a surgeon, who recommended surgery to remove the diseased portion of his bowel.
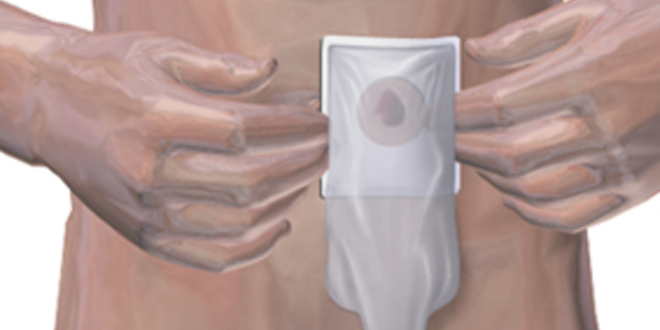
After the surgical procedure, the physician informed William that the diseased portion of the colon was removed and a colostomy had been created. At first, he was angry. How could he continue his active and professional lifestyle? After several days, William began to ask questions about his future, and was taught to fit his ostomy bag device over the stoma by a Certified Ostomy Nurse.
However, he kept thinking about how an ostomy would change everything for him: social interactions, activities, sleep and diet. William was informed that continuing his activities after an ostomy had its challenges, but he would return to normal with education and lifestyle changes.
He began learning the foods he could eat that did not interfere with his activities, as well as how to control odors. Everything progressed well, but on his three-month follow-up visit with the surgeon, he shared that his wife did not want to be intimate with him. This was one area that he did not recognize would be affected by the ostomy.
William then found help through the United Ostomy Associations of America (UOAA) and local UOAA support groups. He and his wife attended these support group meetings and found that their story was not much different from other ostomy patients. The pair learned to discuss the ostomy with friends and. most importantly, how their relationship could continue using tips from a Certified Ostomy Nurse and fellow support group attendees.
There are resources available to individuals and families of ostomy patients. The UOAA is a leading nonprofit organization dedicated to supporting, improving and advocating for those individuals who will have an ostomy, intestinal or urinary diversion. The organization’s website at ostomy.org has ostomy information, a discussion board, conferences, a list of local support groups and the association’s magazine, The Phoenix.
Local UOAA support groups hold two meetings a month. The Jacksonville Chapter meets at 3 p.m. the third Sunday of each month at 4836 Victor St. in San Marco. The Amelia Island Chapter meets at 6:30 p.m. the second Monday of the month at UF Health North, 15255 Max Leggett Parkway, near Oceanway.
Each meeting is attended by those with ostomies who share their success living with an ostomy, and also by a Certified Ostomy Nurse offering professional advice.
Information for Nursed to Health is based on actual and composite cases of patients treated by students, alumni and faculty of Jacksonville University’s Keigwin School of Nursing. Names and specific medical information have been changed to protect private health information, and any similarity is coincidental. For more information about JU’s Keigwin School of Nursing, visit www.ju.edu/nursing. Readers with specific questions regarding their own health concerns should seek the advice of their healthcare provider.
Nursed to Health is an occasional feature in The Florida Times-Union in which Jacksonville University Keigwin School of Nursing faculty discuss symptoms, diagnoses and treatments based on actual and composites of patient cases handled by instructors, students and alumni of JU’s local training programs. Today’s column is by Dennis Oakes, Clinical Assistant Professor of Nursing in JU’s Brooks Rehabilitation College of Healthcare Sciences and a specialist in Critical Care Nursing.
Names and specific medical information in Nursed to Health have been changed to protect private health information, and any similarity is coincidental. For more information about JU’s Keigwin School of Nursing, visit www.ju.edu/chs/nursing. Readers with specific questions regarding their own health concerns should seek the advice of their healthcare provider.
 Wave Magazine Online Jacksonville University News Hub
Wave Magazine Online Jacksonville University News Hub